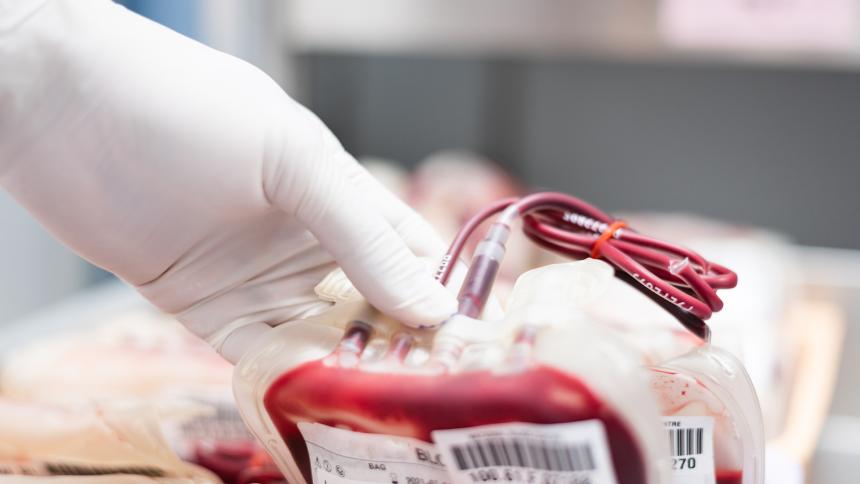
Infected blood scandal: The biggest NHS disaster in history
It’s widely regarded as the biggest treatment disaster in the history of the NHS, but just what is the infected blood scandal, and how did it impact tens of thousands of people across the country?
What happened?
Throughout the 1970s, 80s and early 90s, thousands of people in the UK were infected with HIV and hepatitis C after receiving blood products that were contaminated with the viruses.
Many of those affected were people living with haemophilia and similar disorders where blood is unable to clot properly. Patients can suffer spontaneous internal bleeding, while external injuries that would usually be considered mild can lead to uncontrolled and profuse bleeding.
Haemophilia is caused by a deficiency of either clotting factor VIII or IX, which are proteins in blood plasma. Once upon a time, doctors could only treat patients by way of long, arduous blood transfusions. But that changed in the 1970s with the mass rollout of a revolutionary new treatment: clotting factor concentrate which could be injected by patients at home.
But what patients didn’t realise was that many batches of the miraculous medication were contaminated. It’s estimated that 1,250 people with bleeding disorders in the UK – including 380 children – were infected with both HIV and hepatitis C between 1970 and 1991. Many of these went on to develop, and die from, AIDS.
It’s also estimated that at least 2,400 people with bleeding disorders were solely infected with hepatitis C, a virus which attacks the liver and can cause liver cirrhosis and cancer.
As well as those with bleeding disorders, patients who received blood transfusions after childbirth, surgery and other treatments were also placed in harm’s way during the period. It’s thought that at least 79 (and potentially up to 100) people were infected with HIV through blood transfusions, and at least 21,300 people were infected with hepatitis C.
Why did it happen?
The much-needed clotting factor concentrate was manufactured using industrial quantities of human blood plasma. In the United States, which supplied the UK with much of this medication, it was perfectly legal for pharmaceutical companies to pay people to donate blood, which even then was considered by many to be an unethical practice.
That’s because many people from marginalised and medically higher-risk groups, such as prisoners, drug users, alcoholics and sex workers, were known to repeatedly donate blood to make some quick cash. In her book on the scandal, The Poison Line, journalist Cara McGoogan recounts how inmates in one US prison, who were literally yellow from hepatitis, bribed fellow convicts working in the blood donation centre so they could be allowed to carry on selling their plasma.
Since the manufacture of the medication required pooling plasma from thousands of donors, just one sample infected with HIV/hepatitis C was enough to contaminate an entire batch.
Meanwhile, transfusions in the UK also posed a risk because blood donations weren’t routinely screened for HIV and hepatitis C until 1986 and 1991 respectively.
Who knew?
There were widespread concerns about the safety of blood products even before the HIV/AIDS epidemic began. In 1975, the documentary series World in Action shone a light on how clotting factor concentrate posed a ‘high risk of transmitting hepatitis’, and how drug users, prisoners and others on ‘Skid Row’ were donating much of the plasma being used by the pharmaceutical companies.
The fact that the UK wasn’t producing enough home-grown medication meant that it continued to rely on the controversial US imports. Even after HIV reared its head, the British government was late to acknowledge the risks. In 1983, Ken Clarke – today a Conservative party ‘big beast’, and back then a young health minister – stated that there was ‘no conclusive proof’ that the AIDS virus was transmitted by blood products.
However, by this time many in the medical community had already been sounding the alarm over HIV contamination of blood products. Infectious diseases specialist Dr Spence Galbraith sent a letter to the government warning, ‘all blood products made from blood donated in the USA after 1978 should be withdrawn from use until the risk of AIDS transmission by these products has been clarified.’
Such a ban was ruled out by a committee of government advisors, who believed the benefits to haemophiliacs outweighed the risk of infection.
Speaking about the issue in 2021, Ken Clarke emphasised that the line about a lack of conclusive proof regarding contamination ‘was repeatedly used by every minister… We kept repeating that because that was the scientific advice we had until it was perfectly clear to the medics that there was in fact sufficient proof.’
What next?
A UK-wide public inquiry into the infected blood scandal began taking evidence in 2019. It has gathered powerful testimonies from victims, including former pupils of a Hampshire boarding school which specialised in teaching haemophiliac children. Dozens were given infected blood products with neither the pupils nor their families being told of the risks, and at least 72 died as a result.
The inquiry has witnessed highly controversial moments. Ken Clarke’s defensive testimony regarding his statement of 1983 was branded ‘disgraceful’ by Jason Evans of the campaign group Factor 8, while former prime minister John Major drew gasps from onlookers when he described the scandal as ‘incredibly bad luck’.
The publication of the inquiry report later in 2024 is expected to pave the way for a final, much-delayed compensation deal for the children and parents of those affected. It’s also hoped that the report will finally shed light on how and why a medical calamity of this magnitude unfolded in Britain over such a long period.







